Indigestão
Dispepsia
Revisado por Dr Rachel Hudson, MRCGPÚltima atualização por Dr Philippa Vincent, MRCGPÚltima atualização 21 Ago 2023
Atende aos diretrizes editoriais
- BaixarBaixar
- Compartilhar
- Language
- Discussão
- Versão em Áudio
Nesta série:GastriteDispepsia funcionalÚlcera estomacalÚlcera duodenalHelicobacter pyloriGastroscopia
Dispepsia (indigestão) é um termo que descreve dor e, às vezes, outros sintomas que vêm do trato digestivo superior (o estômago, esôfago ou duodeno). Existem várias causas (descritas abaixo). O tratamento depende da causa provável.
Neste artigo:
Vídeos selecionados para Indigestão e azia
Continue lendo abaixo
O que é indigestão?
Indigestion (dyspepsia) is a term which includes symptoms that come from a problem in the upper gut. The gut (gastrointestinal tract) is the tube that starts at the mouth and ends at the anus. The upper gut includes the oesophagus, stomach and duodenum.
Sintomas de indigestão
Voltar ao conteúdoThe main symptom of indigestion is usually stomach pain or discomfort in the upper abdomen. Other symptoms include:
Inchaço.
Belching.
Sentir-se cheio rapidamente após comer.
Enjoo (náusea).
Vomitar (vômito).
Symptoms are often related to eating. Heartburn (a burning sensation felt in the lower chest area) and bitter-tasting liquid coming up into the back of the throat (sometimes called 'waterbrash') used to be considered as symptoms of dyspepsia. However, these are now considered to be features of a condition called gastro-oesophageal reflux disease (GORD) - see below.
Symptoms tend to occur in bouts which come and go rather than being present all the time. Most people have a bout of dyspepsia, often called indigestion, from time to time - for example, after a large spicy meal. In most cases it soon goes away and is of little concern. However, some people have frequent bouts of dyspepsia which can affect their quality of life.
Continue lendo abaixo
What causes indigestion?
Voltar ao conteúdoCausas comuns
A maioria dos casos de dispepsia repetida (recorrente) deve-se a um dos seguintes:
Dispepsia não ulcerosa. This is sometimes called functional dyspepsia. It means that no cause can be found for the symptoms. It often overlaps with symptoms of irritable bowel syndrome. Consulte o folheto separado chamado Dispepsia Não Ulcerosa (Dispepsia Funcional) para mais detalhes.
Duodenal and stomach (gastric) ulcers. Uma úlcera ocorre quando o revestimento do intestino é danificado e o tecido subjacente fica exposto. Veja os folhetos separados chamados Duodenal Ulcer e Úlcera Estomacal (Úlcera Gástrica) para mais detalhes.
Duodenite e gastrite (inflamação do duodeno e/ou estômago) - que pode ser leve ou mais grave e pode levar a uma úlcera. Veja o folheto separado chamado Gastrite.
Acid reflux, oesophagitis and GORD. Acid reflux occurs when some acid leaks up (refluxes) into the oesophagus from the stomach. See the separate leaflets called Refluxo Ácido e Esofagite e Eosinophilic Oesophagitis para mais detalhes.
Hérnia de hiato. This occurs when the top part of the stomach pushes up into the lower chest through a defect in the diaphragm. See the separate leaflet called Hiatus Hernia for more detail.
A infecção pela bactéria H. pylori - see below.
Medicação. Alguns medicamentos podem causar dispepsia como efeito colateral:
Medicamentos anti-inflamatórios são os culpados mais comuns. Estes são medicamentos que muitas pessoas tomam para artrite, dores musculares, entorses, period pains, etc. Por exemplo: aspirina, ibuprofeno, e diclofenaco - but there are others. Anti-inflammatory medicines sometimes affect the stomach lining and allow acid to cause inflammation and ulcers.
Various other medicines às vezes causam dispepsia, ou pioram a dispepsia. Eles incluem: digoxina, antibióticos, esteroides, ferro, calcium antagonists, nitrates e bisphosphonates.
(Nota: this is not a full list. Check with the leaflet that comes with any medication for a list of possible side-effects.)
H. pylori and dyspepsia
A bacteria called H. pylori can infect the lining of the stomach and duodenum. It is one of the most common infections in the UK. More than 1 in 4 people in the UK become infected with H. pylori at some stage in their lives. Once infected, unless treated, the infection usually stays permanently.
Most people with H. pylori não apresentam sintomas e não sabem que estão infectados. No entanto, H. pylori é a causa mais comum de úlceras duodenais e gástricas. See the separate leaflet called Helicobacter Pylori for more detail.
Outras causas incomuns de dispepsia
Outros problemas do trato digestivo superior, como câncer de estômago e oesophageal cancer, can cause dyspepsia when they first develop.
There are separate leaflets which describe the above conditions in more detail. The rest of this leaflet gives an overview of how dyspepsia is usually managed.
Diagnosticando a indigestão
Voltar ao conteúdoA clinician is likely to do an initial assessment by asking about symptoms and examining the abdomen. The examination is usually normal with any of the common causes of dyspepsia. It is important to review any medicines being taken in case one may be causing the symptoms or making them worse.
Continue lendo abaixo
Como se livrar da indigestão
Voltar ao conteúdoFollowing the initial assessment, depending on the severity and frequency of symptoms, one or more of the following plans of action may be suggested.
Mudanças no estilo de vida
For all types of dyspepsia, the National Institute for Health and Care Excellence (NICE) recommends the following lifestyle changes:
Make sure to eat regular meals.
Stop smoking.
For dyspepsia which is likely to be due to acid reflux, when heartburn is a major symptom, the following may also be worth considering:
Posture. Lying down or bending forwards a lot during the day encourages reflux. Sitting hunched or wearing tight belts may put extra pressure on the stomach, which may make any reflux worse.
Bedtime. If symptoms return most nights, the following may help:
Ir para a cama com o estômago vazio e seco - não comer nas últimas três horas antes de dormir e não beber nas últimas duas horas antes de dormir.
Raising the head of the bed by 10-20 cm (for example, with books or bricks under the mattress or the legs of the bed if this can be done safely). This helps gravity to keep acid from refluxing into the oesophagus.
Antacids taken as required
Antiácidos are alkali liquids or tablets that can neutralise the stomach acid. A dose may give quick relief. There are many brands which can be bought and some are available on prescription. People with mild or infrequent bouts of dyspepsia may find that antacids used when needed are sufficient to manage their symptoms.
A change or alteration in your current medication
This may be possible if a medicine is thought to be causing the symptoms or making them worse.
Test for Helicobacter pylori (H. pylori) infection and treat if it is present
A test to detect H. pylori is commonly done if you have frequent bouts of dyspepsia. As mentioned, it is the underlying cause of most duodenal and stomach ulcers and many cases of gastritis, duodenitis and non-ulcer dyspepsia. This test is via a stool sample. For more information about the diagnosis and treatment of H. pylori, veja o folheto separado chamado Helicobacter Pylori.
Medicamentos para suprimir ácido
A one-month trial of full-dose medication which reduces stomach acid may be considered - in particular, if:
Symptoms are more suggestive of acid reflux or oesophagitis. H. pylori não causa esses problemas.
A infecção pela bactéria H. pylori has been ruled out.
H. pylori has been treated but symptoms persist.
Consulte o folheto separado chamado Medicação para Indigestão para mais informações.
Testes adicionais
Further tests are not needed in most cases. One or more of the above options will usually manage the problem. Reasons why further tests may be advised include:
If additional symptoms suggest that the dyspepsia may be caused by a serious disorder such as stomach or oesophageal cancer or a complication from an ulcer such as bleeding; for example if:
Passing blood with stools (blood can cause black tarry stools).
Bringing up (vomit) blood.
Losing weight unintentionally.
Sentindo-se geralmente indisposto.
Vomiting persistently.
Developing anaemia.
Having an abnormality on examination, such as a lump in the abdomen.
If aged over 55 and develop persistent or unexplained dyspepsia.
If the symptoms are not typical and may be coming from outside the gut, for example, to rule out problems of the gallbladder, pancreas, liver, etc.
If the symptoms are severe and do not respond to treatment.
If there is a risk factor for stomach or oesophageal cancer, such as Esôfago de Barrett, dysplasia, or atrophic gastritis, or had ulcer surgery over 20 years earlier.
Tests advised may include:
Gastroscopy (endoscopy). In this test a clinician looks inside the oesophagus, stomach and duodenum. They do this by passing a thin, flexible telescope down the oesophagus. See the separate leaflet called Gastroscopy (Endoscopy) for more detail.
A blood test to check for anaemia. Anaemia may be due to a bleeding ulcer or to a bleeding stomach cancer. The bleeding might not be noticed if it is not heavy, as the blood can be passed out unnoticed in the stools.
Tests of the gallbladder, pancreas, etc, if the cause of the symptoms is not clear.
Treatment depends on what is found or ruled out by the tests.
Preventing indigestion
Voltar ao conteúdoThe most important factors in preventing indigestion are:
Maintaining a healthy weight.
Not smoking - or stopping smoking.
Drinking alcohol within recommended limits.
Eating a balanced diet.
Eating small regular meals instead of large meals.
Avoiding eating too late at night before going to bed.
Avoiding foods that trigger the indigestion - in some people, they find that certain foods such as onions, garlic, tomatoes or spicy foods will trigger a bout of indigestion. Those people should avoid those triggers.
Understanding digestion
Voltar ao conteúdoO trato digestivo superior
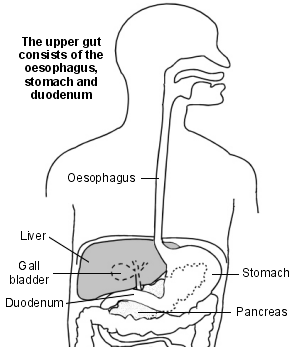
Food passes down the gullet (oesophagus) into the stomach. The stomach makes acid which is not essential but helps to digest food. Food then passes gradually into the first part of the small intestine (the duodenum).
In the duodenum and the rest of the small intestine, food mixes with chemicals called enzymes. The enzymes come from the pancreas and from cells lining the intestine. The enzymes break down (digest) the food. Digested food is then absorbed into the body from the small intestine.
Escolhas do paciente para Indigestão e azia

Saúde digestiva
Reflux ácido e esofagite
Quando o ácido do estômago vaza para o esôfago (tubo que transporta o alimento da boca para o estômago), a condição é conhecida como refluxo ácido. Isso pode causar azia e outros sintomas. Um medicamento que reduz a quantidade de ácido produzido no estômago é um tratamento comum e geralmente funciona bem. Algumas pessoas tomam cursos curtos de medicação quando os sintomas surgem. Algumas pessoas precisam de medicação diária a longo prazo para manter os sintomas afastados.
por Dr. Doug McKechnie, MRCGP

Saúde digestiva
Dispepsia funcional
Functional dyspepsia (non-ulcer dyspepsia) causes pain and sometimes other symptoms in your upper tummy (abdomen). The cause is often not clear. Medication to reduce stomach acid helps in some cases. Infection with Helicobacter pylori (H. pylori) may cause a small number of cases. Clearing this infection, if present, helps in some people.
por Dra. Rosalyn Adleman, MRCGP
Leitura adicional e referências
- Doença do refluxo gastroesofágico e dispepsia em adultos: investigação e manejo; Diretriz Clínica do NICE (setembro de 2014 - última atualização em outubro de 2019)
- Dore MP, Pes GM, Bassotti G, et al; Dyspepsia: When and How to Test for Helicobacter pylori Infection. Gastroenterol Res Pract. 2016;2016:8463614. doi: 10.1155/2016/8463614. Epub 2016 Apr 28.
- Talley NJ, Goodsall T, Potter M; Dispepsia funcional. Aust Prescr. 2017 Dez;40(6):209-213. doi: 10.18773/austprescr.2017.066. Publicado online em 4 de dezembro de 2017.
- Dispepsia - úlcera péptica comprovada; NICE CKS, dezembro de 2022 (acesso apenas no Reino Unido)
- Dispepsia - GORD comprovada; NICE CKS, julho de 2023 (acesso apenas no Reino Unido)
- Dispepsia - funcional comprovada; NICE CKS, dezembro de 2022 (acesso apenas no Reino Unido)
Continue lendo abaixo
Histórico do artigo
As informações nesta página são escritas e revisadas por clínicos qualificados.
Próxima revisão prevista para: 19 Ago 2028
21 Ago 2023 | Última versão

Pergunte, compartilhe, conecte-se.
Navegue por discussões, faça perguntas e compartilhe experiências em centenas de tópicos de saúde.

Sentindo-se mal?
Avalie seus sintomas online gratuitamente
Inscreva-se no boletim informativo do Patient
Sua dose semanal de conselhos de saúde claros e confiáveis - escritos para ajudá-lo a se sentir informado, confiante e no controle.
Ao se inscrever, você aceita nossos Política de Privacidade. Você pode cancelar a inscrição a qualquer momento. Nunca vendemos seus dados.