Pneumonia
Revisado por Dr Toni Hazell, MRCGPÚltima atualização por Dr Mohammad Sharif Razai, MRCGPLast updated 24 Jun 2024
Atende aos diretrizes editoriais
- BaixarBaixar
- Compartilhar
- Language
- Discussão
- Versão em Áudio
Nesta série:Infecção no peitoBronquite agudaPneumonia por aspiraçãoInfecção torácica pós-operatóriaBroncoscopia
Pneumonia is a lung infection that causes inflammation and swelling in the air sacs (alveoli). These sacs can fill with fluid, making it harder to breathe and for oxygen to reach the bloodstream. It's usually caused by bacterial infections but can also be caused by viral infections, and sometimes fungi.
This leaflet explains the types, causes, symptoms, treatment, and prevention of pneumonia.
Neste artigo:
Video picks for Infecções no peito e pulmões
Pontos principais
Pneumonia is a lung infection that causes inflammation and fluid in the air sacs, making breathing difficult.
It is usually caused by bacteria, such as Streptococcus pneumoniae, but can also be caused by viruses (such as flu or COVID-19) or fungi.
Common symptoms include cough, fever, chills, chest pain, tiredness, and shortness of breath. You should seek urgent medical help if your symptoms are severe or breathing is difficult.
Most cases of pneumonia are treated with antibiotics, fluids, and plenty of rest. Severe pneumonia may require hospital admission.
Continue lendo abaixo
O que é pneumonia?
Pneumonia is inflammation of the lungs. Pneumonia can affect one or both lungs, and you can even have it without knowing it. This is sometimes called walking pneumonia.
Anyone can get pneumonia, but it mostly affects people younger than 5 or over the age of 65 due to their weakened immune systems. Smoking and alcohol consumption may also raise your risk of catching pneumonia.
Pneumonia is often more serious than bronchitis, which is the inflammation or infection of the large airways called the bronchi (see diagram). It's possible to have both conditions at the same time, known as bronchopneumonia.
Pneumonia patch diagram
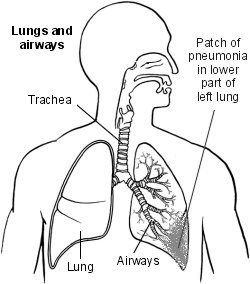
Types of pneumonia
Voltar ao conteúdoPneumonia is usually classified based on where it is acquired. For example, it can be hospital-acquired or community-acquired. Sometimes, it is classified by how the infection is caught, such as aspiration pneumonia.
Pneumonia adquirida no hospital
Hospital-acquired pneumonia is a lung infection that develops at least 48 hours after being admitted to the hospital and was not present when you were admitted. This is different from ventilator-associated pneumonia, which occurs more than 48 hours after a patient has been put on a ventilator.
Hospital acquired pneumonia is more common in patients in the intensive care unit, those who have recently had major surgery, or those who have been in the hospital for a long time. Symptoms usually include fever or low body temperature, thick mucus, and difficulty getting enough oxygen
Pneumonia por aspiração
A particular type of pneumonia is known as pneumonia por aspiração.
This occurs when small amounts of stomach contents or liquids from the mouth or throat are inhaled into the lungs. These inhaled substances can irritate the lungs, cause infection, or block the smaller airways.
Aspiration pneumonia usually affects frail elderly people, those who are drowsy or unconscious, or individuals with conditions that cause swallowing difficulties.
Continue lendo abaixo
Symptoms of pneumonia
Voltar ao conteúdoCommon symptoms of pneumonia include:
Tosse.
Sentindo-se geralmente indisposto.
Uma temperatura alta (febre).
Perda de apetite.
Suor.
Tremendo.
Dores de cabeça.
Dores e desconfortos.
All these symptoms are also seen in gripe (influenza) so it is sometimes difficult to diagnose pneumonia in the early stages. See the separate leaflet called Flu (Influenza) for further details.
How to tell if it's pneumonia or the flu?
Coughing
Coughing up a lot of phlegm (sputum) is more likely to happen in pneumonia than in flu. The phlegm may become yellow-coloured or green-coloured. It may be streaked with blood, or you may cough up more significant amounts of blood.
Falta de ar
You may become short of breath, start breathing faster than normal, and develop a tight chest. If the infection involves the pleura (the membrane between the lung and the chest wall), you might feel a sharp pain in the side of your chest. A doctor may hear crackles when listening to your chest with a stethoscope.
How long does pneumonia last?
Voltar ao conteúdoThe duration of pneumonia depends on the severity of the illness and who gets it. According to the NHS, it may take up to 6 months to feel completely back to normal. However, symptoms should have substantially reduced in mild cases after 4 to 6 weeks.
Continue lendo abaixo
When should you see a doctor for pneumonia?
Voltar ao conteúdoWho you see depends on your symptoms and how unwell you feel. Seek appropriate care based on the severity of your condition. For example, if you experience severe difficulty breathing, chest pain, confusion or disorientation, seek emergency care by calling an ambulance.
If you have asma ou doença pulmonar obstrutiva crônica (DPOC), and feel unwell you should ask your doctor for advice.
Your doctor may recommend increasing your inhaler medication or using a 'rescue pack' of antibiotics and steroid tablets at the first sign of an infection. For those with asthma, this information might be included in your personalised asthma action plan. If it is not, consult your doctor for advice if you develop symptoms of a chest infection.
There are a number of pneumonia symptoms that mean you should see a healthcare professional, including a GP, even if you do not have any other lung problems. They include:
If a fever, wheezing or headache becomes worse or severe.
Se você desenvolver respiração rápida, falta de ar ou dores no peito.
If you cough up blood or if your phlegm becomes dark or rusty-coloured.
Se você ficar sonolento ou confuso.
If a cough lasts for longer than 3-4 weeks.
If you have repeated bouts of acute bronchitis.
Se surgir qualquer outro sintoma que lhe preocupe.
Causes of pneumonia
Voltar ao conteúdoPneumonia is an infection commonly caused by bacteria or viruses. Bacteria causes bacterial pneumonia and viruses cause viral pneumonia.
Streptococcus pneumoniae bacteria is the most common cause in both adults and children. Other bacterial causes include Haemophilus influenzae and Staphylococcus aureus.
Respiratory viruses such as flu, respiratory syncytial virus (RSV), measles virus and coronavirus can cause viral pneumonia, which is usually milder than bacterial pneumonia. However, those with viral pneumonia are at risk of getting bacterial pneumonia.
A well-known group of bacteria called atypicals, such as Mycoplasma pneumoniae and Legionella pneumophila, causes pneumonia in about 3 out of 10 cases. Other germs, such as fungi, yeasts, or protozoa, can sometimes also cause pneumonia.
Rarely, pneumonia can be caused by inhaling poisons or chemicals rather than an infection. Many different substances, including liquids, gases, small particles, dust, or fumes, can cause this.
You may breathe in bacteria, viruses, or other germs. If you are normally healthy, a small number of germs usually does not matter. They will be trapped in your phlegm (sputum) and killed by your immune system. However, sometimes the germs multiply and cause lung infections.
Risk factors for pneumonia
You are more likely to catch pneumonia if you are already in poor health or have certain health conditions, for example:
If you are frail or elderly.
If you have a lung disease such as DPOC.
If you have diabetes.
If you have heart, liver or kidney disease.
If you have neurological conditions that increase the risk of inhaling food or liquids (aspiration).
If you have low immunity to infection (sistema imunológico enfraquecido). Low immunity can be caused by immunosuppressant medications, untreated HIV, or another serious illness.
However, even healthy people sometimes develop pneumonia.
How is pneumonia diagnosed?
Voltar ao conteúdoA doctor will suspect pneumonia by asking about your symptoms. They may also ask about:
Your medical history and that of your family.
Whether you smoke, how much and for how long.
The examination may include:
Verificando sua temperatura.
Listening to your heart and lungs with a stethoscope. They may want to lift or take off your top. If you want a chaperone during the examination, the doctor will arrange one.
Tapping your chest over the infected lung (percussion). An area of an infected lung may sound dull.
Checking how much oxygen is circulating in your body by using a small device called a pulse oximeter. This device is placed on the end of your finger.
Checking your peak flow measurement if you have asthma.
Radiografia de tórax
A raio-X de tórax may be required to confirm the diagnosis and to see how serious the infection is.
Outros exames
These tests are usually carried out if you need to be admitted to hospital. They include sending a sample of phlegm (sputum) for analysis and blood tests to check if the infection has spread to your blood.
Pneumonia treatment
Voltar ao conteúdoYou may need medications to treat your pneumonia, depending on the cause and type of pneumonia.
Medicamentos
Treating pneumonia at home may be sufficient if you are normally healthy and the pneumonia is not severe.
If the doctor thinks you have pneumonia, an antibiotic such as amoxicillin is prescribed. Once pneumonia is diagnosed, it's best to start treatment within four hours and complete the prescribed course. Bacterial infection is a common cause, and antibiotic medications kill bacteria. However, antibiotic medicines don't work against viruses.
Amoxicillin is usually effective against the most common causes. If it doesn't seem to be effective and your doctor suspects a less common bacterial infection, they may change your medication.
If you are allergic to penicillin (amoxicillin is a type of penicillin), your doctor will prescribe an alternative, such as clarithromycin, that works just as well. Antibiotics in capsule, tablet, or liquid form are preferred to injections through a vein (intravenous), provided you can take them.
Antibiotic treatment is usually effective, and you can expect to recover fully. If the treatment is working, symptoms should start to improve after three days. In most cases, antibiotics can be stopped in five days unless you are still very unwell.
Autocuidado
During your recovery, ensure you:
Have lots to drink, to avoid becoming lacking in fluid in the body (dehydrated).
Take regular paracetamol to ease high temperature (fever) and headaches.
Let a doctor know if symptoms do not improve over the following three days.
You may feel tired for a while after the infection has cleared. If the symptoms persist for longer than three weeks, you should ask your doctor to check you again.
Tratamento hospitalar
Hospital admission may be advised if you have severe pneumonia or if symptoms do not quickly improve after you have started antibiotic treatment.
You are more likely to be treated in hospital if you are already in poor health, or if an infection with a more serious infecting germ is suspected. For example, if infection with Legionella pneumophila (the bacterium that causes Doença dos Legionários) is suspected.
Even if you are in hospital, you are likely to be offered antibiotics in capsule, tablet or liquid form unless you have difficulties taking them, in which case they may be given through a vein. If the condition is thought to be severe, you may only be given antibiotics through a vein. Your antibiotic treatment will be stopped after five days, unless you are very unwell.
Sometimes oxygen and other supportive treatments are needed if you have severe pneumonia. Those who become severely unwell may need treatment in an intensive care unit or high dependency unit.
When you return home, even though the infection is treated, you may feel tired and unwell for some time.
Complicações da pneumonia
Voltar ao conteúdoPneumonia can cause complications, especially in people with existing health conditions, those who are frail, or patients with weakened immune systems.
Potential complications include:
Fluid buildup around the lungs can occur in the pleura, which are thin membranes lining the lungs and the inside of the chest wall. This condition is called pleural effusion and can cause chest pain and difficulty breathing. It is often necessary to drain the excess fluid, especially if it is infected.
Pus formation in the lung (lung abscess). This may need treatment with antibiotics or drainage through a needle or surgery.
Infection spreads to the bloodstream (bacteraemia). This serious condition can lead to sepsis, causing a drop in blood pressure and damage to various organs.
Severe lung inflammation and fluid buildup (acute respiratory distress syndrome). This is a life-threatening condition that requires urgent medical care.
Pus collects in the space between the lungs and the chest wall (ampyema). This condition often requires the pus to be drained with a needle or surgery to prevent the infection from spreading.
Infection can strain the kidneys, heart or liver. Pneumonia can worsen existing health conditions, leading to complications such as kidney failure or heart attacks.
How to prevent pneumonia
Voltar ao conteúdoCertain protective measures can help prevent some types of pneumonia or reduce the severity and duration of the illness. These include:
Vacinação
One of the most effective ways to prevent pneumonia is through immunisation against pneumococcus, the most common cause of bacterial pneumonia.
Getting the annual flu vaccine can also help prevent pneumonia. The flu jab is especially recommended if you are 65 years or older, have a health condition, are pregnant, or are a young child.
Babies should also be vaccinated against Hib (Haemophilus influenzae type b) as part of their imunizações infantis de rotina.
Consulte os folhetos separados chamados Imunização pneumocócica e Imunização contra a gripe (Vacina da gripe) for further details.
Mudanças no estilo de vida
Other prevention measures include maintaining a healthy lifestyle and washing hands with soap and water for 20 seconds. Cigarette smoke damages the lining of the airways and makes the lungs more prone to infection. Therefore, parar de fumar will reduce your risk of developing lung infections.
Perguntas frequentes
Voltar ao conteúdoIs pneumonia contagious?
Pneumonia can be contagious, depending on the cause. Bacterial and viral pneumonia can spread through coughs, sneezes, or by touching contaminated surfaces. However, not everyone exposed to these germs will develop pneumonia.
Is pneumonia deadly?
Pneumonia can be deadly, especially in older adults, people with weak immune systems, or severe cases needing hospital care. Most healthy people recover well at home, with deaths being rare.
Can pneumonia go away on it's own?
Mild cases of viral pneumonia can clear up on it's own with rest and fluids, but bacterial pneumonia usually needs antibiotics. Without treatment, pneumonia can get worse and cause serious complications.
Patient picks for Infecções no peito e pulmões

Tórax e pulmões
Tuberculose
Tuberculosis (TB) is an infection with a germ (bacterium) called Mycobacterium tuberculosis. If you have symptoms, or a doctor can find signs of the infection when examining you, this is known as active tuberculosis. If you have TB infection without any signs or symptoms, this is known as latent TB.
por Dr. Colin Tidy, MRCGP

Tórax e pulmões
Vírus SARS e MERS
Síndrome respiratório agudo grave (SRAG) e síndrome respiratória do Oriente Médio (MERS) são infecções virais. Ambas podem causar doenças muito graves que afetam principalmente os pulmões. O SRAG causou muitas infecções, especialmente na Ásia, entre 2002 e 2004, mas ficou sem notícias por algum tempo. Um surto de SARS-CoV-2 (COVID-19) surgiu em Wuhan, China, em dezembro de 2019. Isso se espalhou rapidamente e foi declarado uma pandemia global em 2020. O MERS foi reconhecido pela primeira vez no Oriente Médio em 2012. A maioria das infecções iniciais ocorreu no Oriente Médio. No entanto, até fevereiro de 2018, a Organização Mundial da Saúde (OMS) havia relatado casos em muitos outros países.
by Dr Hayley Willacy, FRCGP
Leitura adicional e referências
- Pneumonia: Diagnóstico e manejo da pneumonia adquirida na comunidade e no hospital em adultos; Diretriz Clínica NICE (Dezembro de 2014 - última atualização em outubro de 2023)
- Tosse (aguda): prescrição de antimicrobianos; Orientação NICE (Fevereiro de 2019)
- Pneumonia (adquirida na comunidade): prescrição de antimicrobianos; Orientação NICE (setembro de 2019)
- Pneumonia (adquirida no hospital): prescrição de antimicrobianos; Orientação NICE (setembro de 2019)
- Diretriz BTS Anotada para o manejo de PAC em adultos; Sociedade Torácica Britânica (2009 - Resumo das recomendações atualizado em 2015)
- Torres A, Peetermans WE, Viegi G, et al; Fatores de risco para pneumonia adquirida na comunidade em adultos na Europa: uma revisão da literatura. Thorax. 2013 Nov;68(11):1057-65. doi: 10.1136/thoraxjnl-2013-204282.
- Metlay JP, Waterer GW, Long AC, et al; Diagnosis and Treatment of Adults with Community-acquired Pneumonia. An Official Clinical Practice Guideline of the American Thoracic Society and Infectious Diseases Society of America. Am J Respir Crit Care Med. 2019 Oct 1;200(7):e45-e67. doi: 10.1164/rccm.201908-1581ST.
Continue lendo abaixo
Histórico do artigo
As informações nesta página são escritas e revisadas por clínicos qualificados.
Próxima revisão prevista para: 24 Jun 2027
24 Jun 2024 | Última versão

Pergunte, compartilhe, conecte-se.
Navegue por discussões, faça perguntas e compartilhe experiências em centenas de tópicos de saúde.

Sentindo-se mal?
Avalie seus sintomas online gratuitamente
Inscreva-se no boletim informativo do Patient
Sua dose semanal de conselhos de saúde claros e confiáveis - escritos para ajudá-lo a se sentir informado, confiante e no controle.
By subscribing you accept our Política de Privacidade. Você pode cancelar a inscrição a qualquer momento. Nunca vendemos seus dados.