Psoríase das mãos e pés
Revisado por Dr Rosalyn Adleman, MRCGPÚltima atualização por Dr Colin Tidy, MRCGPLast updated 23 Fev 2023
Atende aos diretrizes editoriais
- BaixarBaixar
- Compartilhar
- Language
- Discussão
- Versão em Áudio
- Add to preferred sources on Google
Profissionais de Saúde
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Psoríase article more useful, or one of our other artigos de saúde.
Neste artigo:
Synonyms: psoriasis palmoplantaris, psoriasis palmaris et plantaris
Psoriasis predominantly affecting the palms and soles takes two forms:
Erythematous scaly plaques typical of psoriasis elsewhere in the body.
More generalised thickening and scaling (keratoderma).
Palmoplantar pustulosis (PPP) is a chronic, recurrent skin disease belonging to the spectrum of psoriasis. It is characterised by an eruption of sterile pustules on the palms and soles.1 See the 'Palmoplantar pustulosis' section at the end of this article.
Veja também o separado Doença Ungueal Psoriática artigo.
Continue lendo abaixo
How common is psoriasis? (Epidemiology)2
Psoriasis is common, but its prevalence and incidence may be underestimated, as people with mild psoriasis may not consult healthcare professionals. There is considerable variation in the estimates of psoriasis prevalence between populations and countries. Around 1-3% of the world's population are estimated to have psoriasis. About 1.3-2.8% of the UK population are estimated to have psoriasis.
Both the incidence and prevalence of psoriasis has been shown to increase with increasing latitude in the UK.
Onset may occur at any age, but there are two peaks in incidence, between 20-30 years of age, and 50-60 years of age. Psoriasis is uncommon in children, with most studies indicating an estimated prevalence of less than 0.5%.
Men and women are equally affected, but localised pustular psoriasis is more common in women than in men.
White people are more likely to develop the condition compared with other ethnic groups.
A positive family history may exist for 40-50% of people with psoriasis, and this may be up to 75% in people with early life onset.
Aparência visual
Voltar ao conteúdoPsoríase nas mãos
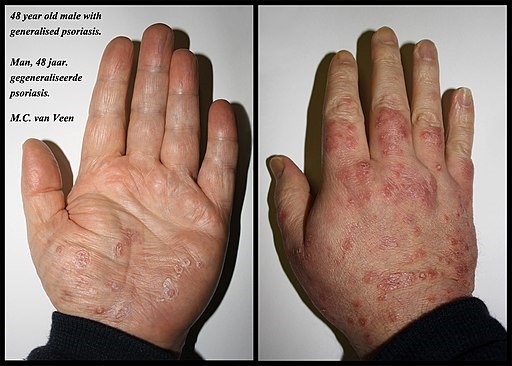
© MCvanVeen, CC BY-SA 4.0 via Wikimedia Commons
Continue lendo abaixo
Psoriasis symptoms
Voltar ao conteúdoRed scaly plaques.
Hyperkeratotic areas.
Central palm or weight-bearing areas of the soles.
Well demarcated.
Painful cracking and fissuring.
Diagnóstico diferencial
Voltar ao conteúdoHyperkeratotic eczema.
Palmoplantar pustulosis (PPP) (see section below).
Continue lendo abaixo
Psoriasis treatment and management
Voltar ao conteúdoVeja também o separado Psoríase em Placas Crônicas artigo.
Gestão em cuidados primários
Classical psoriatic lesions can be treated with a vitamin D ointment (calcipotriol/Dovonex® or tacalcitol/Curatoderm®) or dithranol (Dithrocream®/Micanol®).
In palm and sole psoriasis, both hyperkeratosis and inflammation are usually present and may require separate treatments:
Hyperkeratosis usually needs to be treated with a keratolytic agent such as 2% salicylic acid ointment BP.
This can be alternated morning and evening with a topical steroid (usually potent, due to the thick skin at this site).3
Quando encaminhar2
Where there is diagnostic uncertainty.
For further patient counselling and education.
Where topical treatment has failed, or treatment has not been tolerated.
Where there is significant physical, psychological, social or occupational difficulty.
Tratamentos adicionais
Further treatment options in secondary care include low doses of oral retinoids with psoralen combined with ultraviolet A (PUVA) or UVB phototherapy, methotrexate, ciclosporin or acitretin. Calcineurin inhibitors such as tacrolimus or pimecrolimus and biological agents such as infliximab and alefacept have been used with some success.4
Complicações
Voltar ao conteúdoPain can restrict the use of hands or walking.
Prognóstico
Voltar ao conteúdoPsoriasis of the hands and feet tends to be persistent and, in some, quite resistant to treatment.
Palmoplantar pustulosis3
Voltar ao conteúdoPalmoplantar pustulosis (PPP) most often occurs in middle-aged women. Painful skin lesions appear on the hands and feet, significantly reducing quality of life. The pathogenesis is poorly understood, although it is known that genetic, immunological and environmental factors play a role in its development. Clinical observations confirm the role of nicotine and contact allergens in the development of the lesions. The skin lesions can also occur as a side effect of certain medications. In some cases, PPP coexists with other diseases, such as seronegative arthropathies, coeliac disease and thyroid diseases. There is also a connection with infectious bacterial foci. Exacerbation of the skin lesions is triggered by stress.5
Palmoplantar pustulosis epidemiology
The prevalence of PPP is estimated to range from 0.01 to 0.05%. It is more common in people with a family history of psoriasis and trigger factors include smoking, infection, stress and some drugs, particularly anti-tumor necrosis factor (TNF) agents.1
Apresentação
PPP typically presents as multiple sterile pustules on the palms and soles (initially yellowish fading to brown macular pinpoint lesions).
Psoriasis of the feet
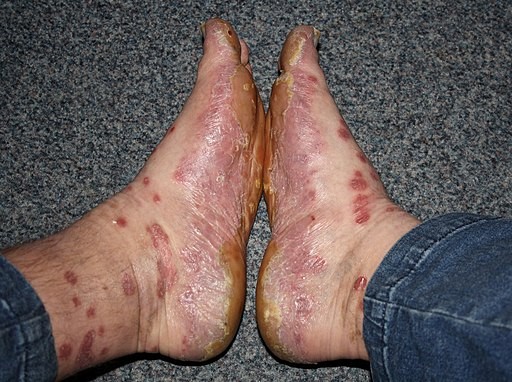
© MCvanVeen, CC BY-SA 4.0, via Wikimedia Commons
Affected areas may become red, scaly and frequently painful. Eruptions of pustules occur unpredictably and may return repeatedly over years.
Diagnóstico diferencial
Infected eczema - less defined, white vesicles rather than pustules, swabs often grow Staphylococcus aureus.
Acute pompholyx is an episodic form of eczema affecting the palms and soles with bullae formation, which frequently becomes infected.
Tinea pedis - commonly unilateral or asymmetrical erythema, scaling and pustules. Toe clefts and nails are usually involved.
Artrite reativa - gross palmar and plantar lesions may occur (keratoderma blennorrhagica) which are histologically indistinguishable from psoriasis. This also affects the mouth and penis.
Acrodermatitis continua of Hallopeau (ACH): a rare indolent form of psoriasis with sterile pustular changes and dactylitis affecting the distal digits and nails.6
Gestão em cuidados primários3 7
Treatment of palmoplantar pustulosis does not cure the disorder and is not always successful.
Encourage general measures:
Cessação do tabagismo.
Good footwear made from natural fibres.
Avoidance of even minor trauma.
Waterproof dressings over fissured areas.
Resting the affected area where possible.
Emollients are important:
Apply thick greasy emollients to soften skin and prevent fissures.
Soak in warm water with emulsifying ointment.
Use salicylic acid ointment or urea cream to peel dead skin.
Wash with soap substitutes.
Potent topical steroid ointments - eg, clobetasol propionate - may be used twice daily for limited periods. High-potency steroids are required in order to penetrate the thick skin of the hands and feet. Occlusion with cling film or dressings can enhance penetration but should not be used for more than five days in a row.
Coal tar is messy but can be applied directly, often mixed into an ointment base.
Oral acitretin.
Narrow-band UVB and photochemotherapy. The combination of exposure to ultraviolet radiation (UV-A) with psoralens taken as tablets or applied topically can be very effective. Careful supervision is necessary to avoid burning.
A variety of other medications can sometimes help, including colchicine, dapsone, methotrexate, tetracyclines and ciclosporin.
Quando encaminhar3
Referral is primarily for help with diagnosis and treatment, or if symptoms are particularly disabling.
Palms and soles are difficult sites to treat and PPP can be resistant to treatment so specialist advice may be required.
Tratamentos adicionais8
Further treatment options which dermatologists can use include:
Systemic retinoids - for example, acitretin, arotinoid ethyl ester.
PUVA treatment to hands and feet (sometimes combined with systemic retinoids).
Metotrexato.3
Etanercept is sometimes used. A good response to a combination of etanercept and alitretinoin has been reported.9
Phototherapy and ciclosporin have also been found helpful.
Complicações
Pain from lesions and associated fissuring may be significant.
Walking and standing for long periods can exacerbate lesions on the soles of the feet.
Manual activity can be uncomfortable if the hands are affected.
Occupational and functional disability secondary to above.
Pustulotic arthro-osteitis (sterile inflammatory osteitis of the sternoclavicular region) is a rare but severe complication of palmar pustulosis.10
Prognóstico
The condition tends to be chronic and poorly responsive to treatment.3
Leitura adicional e referências
- Psoriasis Palmoplantaris; DermIS (Sistema de Informação em Dermatologia)
- Pustular Psoriasis of the Palms and Soles; DermIS (Sistema de Informação em Dermatologia)
- Pustular Psoriasis; Psoriasis Association
- Palmoplantar Pustulosis, DermNet NZ
- Psoríase; DermNet NZ
- Pustular Psoriasis; DermNet NZ
- Psoríase - Caminho de Tratamento na Atenção Primária; Sociedade de Dermatologia de Cuidados Primários, set 2017
- Misiak-Galazka M, Zozula J, Rudnicka L; Palmoplantar Pustulosis: Recent Advances in Etiopathogenesis and Emerging Treatments. Am J Clin Dermatol. 2020 Jun;21(3):355-370. doi: 10.1007/s40257-020-00503-5.
- Psoríase; NICE CKS, setembro de 2022 (acesso apenas no Reino Unido)
- Palmoplantar Pustulosis, DermNet NZ
- Engin B, Askin O, Tuzun Y; Palmoplantar psoriasis. Clin Dermatol. 2017 Jan - Feb;35(1):19-27. doi: 10.1016/j.clindermatol.2016.09.004. Epub 2016 Sep 10.
- Putra-Szczepaniak M, Maj J, Jankowska-Konsur A, et al; Palmoplantar pustulosis: Factors causing and influencing the course of the disease. Adv Clin Exp Med. 2020 Jan;29(1):157-163. doi: 10.17219/acem/112613.
- Di Costanzo L, Napolitano M, Patruno C, et al; Acrodermatitis continua of Hallopeau (ACH): two cases successfully treated with adalimumab. J Dermatolog Treat. 2014 Dec;25(6):489-94. doi: 10.3109/09546634.2013.848259. Epub 2013 Nov 12.
- Raposo I, Torres T; Palmoplantar Psoriasis and Palmoplantar Pustulosis: Current Treatment and Future Prospects. Am J Clin Dermatol. 2016 Aug;17(4):349-58. doi: 10.1007/s40257-016-0191-7.
- Sevrain M, Richard MA, Barnetche T, et al; Treatment for palmoplantar pustular psoriasis: systematic literature review, evidence-based recommendations and expert opinion. J Eur Acad Dermatol Venereol. 2014 Aug;28 Suppl 5:13-6. doi: 10.1111/jdv.12561.
- Meyer V, Goerge T, Luger TA, et al; Successful treatment of palmoplantar hyperkeratotic psoriasis with a combination of etanercept and alitretinoin. J Clin Aesthet Dermatol. 2011 Apr;4(4):45-6.
- Yamamoto T; Pustulotic arthro-osteitis associated with palmoplantar pustulosis. J Dermatol. 2013 Nov;40(11):857-63. doi: 10.1111/1346-8138.12272. Epub 2013 Oct 16.
Continue lendo abaixo
About the author

Dr Colin Tidy, MRCGP
Médico Generalista, Autor Médico
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy é um médico do NHS, baseado em Oxfordshire.
About the reviewerView full bio

Dra. Rosalyn Adleman, MRCGP
MRCGP
A Dra. Rosalyn Adleman é uma médica do NHS que trabalha no norte de Londres.
Histórico do artigo
As informações nesta página são escritas e revisadas por clínicos qualificados.
Próxima revisão prevista: 22 Fev 2028
23 Fev 2023 | Última versão

Pergunte, compartilhe, conecte-se.
Navegue por discussões, faça perguntas e compartilhe experiências em centenas de tópicos de saúde.

Sentindo-se mal?
Avalie seus sintomas online gratuitamente