Dermatite herpetiforme
Revisado por Dr Krishna Vakharia, MRCGPÚltima atualização por Dr Doug McKechnie, MRCGPLast updated 17 Dec 2022
Atende aos diretrizes editoriais
- BaixarBaixar
- Compartilhar
- Language
- Discussão
- Versão em Áudio
- Add to preferred sources on Google
Profissionais de Saúde
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Dermatite herpetiforme article more useful, or one of our other artigos de saúde.
Neste artigo:
Continue lendo abaixo
What is dermatitis herpetiformis?
Dermatitis herpetiformis (DH) is an autoimmune blistering skin disease associated with coeliac disease (gluten enteropathy). DH may be considered as a cutaneous manifestation of coeliac disease.
How common is dermatitis herpetiformis? (Epidemiology)1
Voltar ao conteúdoFor coeliac disease, UK prevalence is around 1%.
However, dermatitis herpetiformis is far more uncommon, affecting between 11.5 and 75 per 100,000.
The most common age of onset is between the third and fourth decade, although the condition may occur at any age after weaning.2
Male patients are affected twice as often as female patients.
Dermatitis herpetiformis predominately affects people of Northern European descent.
Many cases are still under-diagnosed. Diagnosis is challenging, and is frequently delayed by months to years.
The incidence of dermatitis herpetiformis is decreasing, whereas the incidence of coeliac disease is increasing; this may reflect greater awareness and earlier diagnosis of coeliac disease (including via increased use of serological screening), leading to less time for dermatitis herpetiformis to develop.3
Continue lendo abaixo
Dermatitis herpetiformis causes (aetiology)
Voltar ao conteúdoAlthough about 80% of those with dermatitis herpetiformis show histopathological changes of coeliac disease on small intestinal biopsy, only 20% of these patients initially have symptoms of coeliac disease.4
Around 17% of patients with coeliac disease have DH.5
DH may be the first presentation of coeliac disease is some cases.
As in coeliac disease, the core pathogenic mechanisms of DH are thought to be mediated by immunoglobulin A class autoantibodies against one of several transglutaminase enzymes.6
Around 10% of patients have other autoimmune conditions, particularly autoimmune thyroid diseases, anemia perniciosa, gastric atrophy, type I diabetes, lúpus eritematoso sistêmico, Síndrome de Sjögren, sarcodose, vitiligo e alopecia areata.
Sintomas
Voltar ao conteúdoDermatitis herpetiformis is an intensely itchy bullous rash characterised clinically by grouped vesicles on an erythematous base. It characteristically affects extensor surfaces, particularly the scalp, buttocks, elbows and knees. However, lesions can occur on any area of skin.
The lesions are papules and blisters, up to 1 cm in diameter, which are extremely itchy. They arise on normal or reddened skin. Burning, stinging and intense pruritus can precede the appearance of new lesions.
Lesions tend to grow in a centrifugal pattern, with vesicles predominating in the periphery.
The severity can vary from week to week.
Lesions rarely resolve without specific treatment.
NB: primary lesions often are absent owing to the intense, associated pruritus. Instead, many cases present only with erythematous erosions with numerous overlying excoriations.6
Dermatitis herpetiformis rash
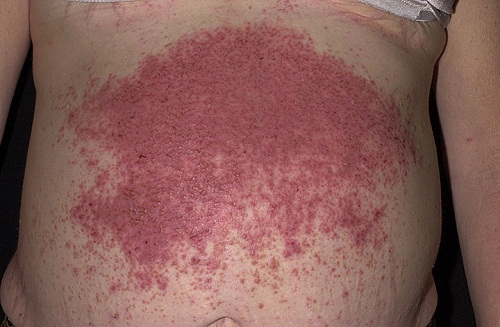
© Madhero88, CC BY-SA 3.0, via Wikimedia Commons
There may also be symptoms of doença celíaca.
Continue lendo abaixo
Investigações
Voltar ao conteúdoBiópsia de pele
The major diagnostic criterion for diagnosis is the presence of granular IgA deposits in the dermal papillae of uninvolved perilesional skin as shown by direct immunofluorescence, and the diagnosis should not be made unless this has been confirmed.2
Testing for coeliac disease
Diagnosis of coeliac disease is by serology and duodenal biopsy, ideally with the patient on a normal - that is, gluten-containing - diet.
IgA anti-tissue transglutaminase or IgA endomysial antibodies are highly specific and sensitive for untreated coeliac disease.4 They are also relevant to dermatitis herpetiformis patients.
Because of their low sensitivity and specificity, antigliadin antibodies are no longer recommended for initial testing.
Biopsy remains essential for the diagnosis of adult coeliac disease and cannot be replaced by serology.2
Outras possíveis investigações
If serology supports the diagnosis of coeliac disease, useful additional blood tests, including FBC, a blood film, haematinics (vitamin B12, folate, ferritin) and U&Es may highlight deficiencies secondary to intestinal malabsorption.7
TFTs are also necessary because of the association of thyroid disease with both coeliac disease and dermatitis herpetiformis.
Investigations for other autoimmune diseases are often necessary.
Diagnóstico diferencial
Voltar ao conteúdoThe presence of plaques (psoriasis), interdigital burrows (scabies), or mucosal blistering (pemphigus) usually suggest an alternative diagnosis.7
Herpes gestationis.
Neurotic excoriations.
Transient acantholytic dermatosis.
Dermatitis herpetiformis treatment
Voltar ao conteúdoA strict gluten-free diet
This is important in order to:
Reduce the medication needed to control skin symptoms. It may be possible to discontinue dapsone when on a gluten-free diet for sufficient time.
Reduce the associated enteropathy, and improve nutrition and bone density.
Tratamento medicamentoso
Dapsone is first choice in cases refractory to dietary management alone and reduces the itch within a day or two.6
Dapsone does not have any effect on intestinal disease.8
Patients taking dapsone should be counselled about the risks associated with dapsone, which include haemolytic anaemia, agranulocytosis, methaemoglobinaemia, and peripheral neuropathy.7 Regular FBCs are necessary.
Sulfapyridine is usually used as an alternative for those cases that do not improve with dapsone.
Complicações
Voltar ao conteúdoComplications may arise from problems associated with coeliac disease. These include:
Neurological problems - ataxia (gluten ataxia), peripheral neuropathy, and epilepsy.
Cardiac problems - pericarditis and cardiomyopathy.
Osteoporosis and poor dental enamel.9
Aphthous ulcers.
Dermatitis herpetiformis shares with coeliac disease an increased risk of developing lymphomas but this seems to be confined to those with severe gut involvement. The risk similarly declines with time on a strict gluten-free diet.2
Prognóstico
Voltar ao conteúdoUntreated, dermatitis herpetiformis follows a prolonged course over years, with relapses and remissions.
The prognosis is good, as dermatitis herpetiformis responds well to diet and medication:
About 80% of patients with dermatitis herpetiformis have good results from a gluten-free diet. The recovery rate varies and some patients can take up to four years to respond.
More than 70% of patients on a strict gluten-free diet are able to slowly wean off dapsone slowly over a period of 24 months.2
Leitura adicional e referências
- Plotnikova N, Miller JL; Dermatitis herpetiformis. Skin Therapy Lett. 2013 Mar-Apr;18(3):1-3.
- Ludvigsson JF, Bai JC, Biagi F, et al; Diagnóstico e manejo da doença celíaca em adultos: diretrizes da Sociedade Britânica de Gastroenterologia. Gut. 2014 Ago;63(8):1210-28. doi: 10.1136/gutjnl-2013-306578. Epub 2014 Jun 10.
- Reunala T, Hervonen K, Salmi T; Dermatitis Herpetiformis: An Update on Diagnosis and Management. Am J Clin Dermatol. 2021 May;22(3):329-338. doi: 10.1007/s40257-020-00584-2.
- Pelkowski TD, Viera AJ; Celiac disease: diagnosis and management. Am Fam Physician. 2014 Jan 15;89(2):99-105.
- Salmi TT, Hervonen K, Kurppa K, et al; Celiac disease evolving into dermatitis herpetiformis in patients adhering to normal or gluten-free diet. Scand J Gastroenterol. 2015 Apr;50(4):387-92. doi: 10.3109/00365521.2014.974204. Epub 2015 Feb 1.
- Yost JM, Hale CS, Meehan SA, et al; Dermatitis herpetiformis. Dermatol Online J. 2014 Dec 16;20(12). pii: 13030/qt4kg43857.
- Jakes AD, Bradley S, Donlevy L; Dermatitis herpetiformis. BMJ. 2014 Apr 16;348:g2557. doi: 10.1136/bmj.g2557.
- Clarindo MV, Possebon AT, Soligo EM, et al; Dermatitis herpetiformis: pathophysiology, clinical presentation, diagnosis and treatment. An Bras Dermatol. 2014 Nov-Dec;89(6):865-75; quiz 876-7.
- Lorinczy K, Juhasz M, Csontos A, et al; Does dermatitis herpetiformis result in bone loss as coeliac disease does? A cross sectional study. Rev Esp Enferm Dig. 2013 Apr;105(4):187-193.
Continue lendo abaixo
About the author

Dr Doug McKechnie, MRCGP
Redator Médico
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
O Dr. Doug McKechnie é um médico do NHS que trabalha em Londres. Ele trabalha em tempo integral na prática clínica e também é o Vice-Líder do módulo de Prática Clínica e Profissional na Faculdade de Medicina da University College London.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr. Krishna Vakharia é uma médica de clínica geral do NHS. Ela também é examinadora regular do Diploma de Pós-Graduação em Dermatologia Prática na Universidade de Cardiff, além de ser a Diretora Médica de Saúde na Optum UK.
Histórico do artigo
As informações nesta página são escritas e revisadas por clínicos qualificados.
Próxima revisão prevista: 15 Nov 2027
17 Dec 2022 | Última versão

Pergunte, compartilhe, conecte-se.
Navegue por discussões, faça perguntas e compartilhe experiências em centenas de tópicos de saúde.

Sentindo-se mal?
Avalie seus sintomas online gratuitamente